Basic ECG Part III
P Wave & PR Interval
Credit To Dr Rayney Azmi Bin Ali
++Characteristics Of The
Normal Sinus P Wave++
Morphology
Smooth
contour
Monophasic
in lead II
Biphasic
in V1
Axis
Normal
P wave axis is between 0° and +75°
P
waves should be upright in leads I and II, inverted in aVR
Duration
*<
120 ms
Amplitude
*<
2.5 mm in the limb leads,
*<
1.5 mm in the precordial leads
Atrial abnormalities are
most easily seen in the inferior leads (II, III and aVF) and lead V1, as the P waves
are most prominent in these leads.
The Atrial Waveform-Relationship
To The P Wave
*Atrial
depolarisation proceeds sequentially from right to left, with the right atrium
activated before the left atrium.
*The
right and left atrial waveforms summate to form the P wave.
*The
first 1/3 of the P wave corresponds to right atrial activation, the final 1/3
corresponds to left atrial activation; the middle 1/3 is a combination of the
two.
*In
most leads (e.g. lead II), the right and left atrial waveforms move in the same
direction, forming a monophasic P wave.
*However,
in lead V1 the right and left atrial waveforms move in opposite directions.
This produces a biphasic P wave with the initial positive deflection
corresponding to right atrial activation and the subsequent negative deflection
denoting left atrial activation.
*This
separation of right and left atrial electrical forces in lead V1 means that
abnormalities affecting each individual atrial waveform can be discerned in
this lead. Elsewhere, the overall shape of the P wave is used to infer the
atrial abnormality.
First Degree AV Block Vs Second Degree Mobitz Type I (Wenckebach)
++First Degree AV Block++
Causes of First Degree AV Block
*Increased vagal tone
*Athletic training
*Inferior MI
*Mitral valve surgery
*Myocarditis (e.g. Lyme disease)
*Electrolyte disturbances (e.g. Hyperkalaemia)
*AV nodal blocking drugs (beta-blockers, calcium channel blockers, digoxin,
amiodarone)
*May be a normal variant
++Second Degree Mobitz Type I (Wenckebach)++
Definition Of Wenckebach Phenomenon:
*Progressive prolongation of the PR interval culminating in
a non-conducted P wave.
*The PR interval is longest immediately before the dropped
beat.
*The PR interval is shortest immediately after the dropped
beat.
Other Features Of Second Degree Mobitz Type I
*The P-P interval remains relatively constant.
*The greatest increase in PR interval duration is typically
between the first and second beats of the cycle.
*The R-R interval progressively shortens with each beat of
the cycle.
*The Wenckebach pattern tends to repeat in P:QRS groups
with ratios of 3:2, 4:3 or 5:4.
Mechanism
*Mobitz I is usually due to reversible conduction lock at
the level of the AV node.
*Malfunctioning AV node cells tend to progressively fatigue
until they fail to conduct an impulse.
*This is different to cells of the His-Purkinje system
which tend to fail suddenly and
unexpectedly (i.e. producing a Mobitz II block).
Causes of Wenckebach Phenomenon
*Drugs: beta-blockers, calcium channel blockers, digoxin,
amiodarone
*Increased vagal tone (e.g. athletes)
*Inferior MI
*Myocarditis
*Following cardiac surgery (mitral valve repair, Tetralogy of
Fallot repair)
Clinical Significance of AV Block: Second Degree,
Mobitz I
*Mobitz I is usually a benign rhythm, causing
minimal haemodynamic disturbance and with low risk of progression to third
degree heart block.
*Asymptomatic patients do not require
treatment.
*Symptomatic patients usually respond to
atropine.
*Permanent pacing is rarely required.
++Second Degree Mobitz Type II++
AV
Block: 2nd degree, Mobitz II Overview
*Intermittent
non-conducted P waves without progressive prolongation of the PR interval
(compare this to Mobitz I).
*The
PR interval in the conducted beats remains constant.
*The
P waves ‘march through’ at a constant rate.
*The
RR interval surrounding the dropped beats is an exact multiple of the preceding
RR interval (e.g. double the preceding RR interval for a single dropped beat,
treble for two dropped beats, etc)
Mechanism
*Mobitz
II is usually due to failure of conduction at the level of the His-Purkinje
system (i.e. below the AV node).
*While
Mobitz I is usually due to a functional suppression of AV conduction (e.g. due
to drugs, reversible ischaemia), Mobitz II is more likely to be due to
structural damage to the conducting system (e.g. infarction, fibrosis,
necrosis).
*Patients
typically have a pre-existing LBBB or bifascicular block, and the 2nd degree AV
block is produced by intermittent failure of the remaining fascicle (“bilateral
bundle-branch block”).
*In
around 75% of cases, the conduction block is located distal to the Bundle of
His, producing broad QRS complexes.
*In
the remaining 25% of cases, the conduction block is located within the His
Bundle itself, producing narrow QRS complexes.
*Unlike
Mobitz I, which is produced by progressive fatigue of the AV nodal cells,
Mobitz II is an “all or nothing” phenomenon whereby the His-Purkinje cells
suddenly and unexpectedly fail to conduct a supraventricular impulse.
*There
may be no pattern to the conduction blockade, or alternatively there may be a
fixed relationship between the P waves and QRS complexes, e.g. 2:1 block, 3:1
block.
Causes
of Mobitz II
*Anterior
MI (due to septal infarction with necrosis of the bundle branches).
*Idiopathic
fibrosis of the conducting system (Lenegre’s or Lev’s disease).
*Cardiac
surgery (especially surgery occurring close to the septum, e.g. mitral valve
repair)
*Inflammatory
conditions (rheumatic fever, myocarditis, Lyme disease).
*Autoimmune
(SLE, systemic sclerosis).
*Infiltrative
myocardial disease (amyloidosis, haemochromatosis, sarcoidosis).
*Hyperkalaemia.
*Drugs:
beta-blockers, calcium channel blockers, digoxin, amiodarone.
Clinical
Significance
*Mobitz
II is much more likely than Mobitz I to be associated with haemodynamic
compromise, severe bradycardia and progression to 3rd degree heart block.
*Onset
of haemodynamic instability may be sudden and unexpected, causing syncope
(Stokes-Adams attacks) or sudden cardiac death.
*The
risk of asystole is around 35% per year.
*Mobitz
II mandates immediate admission for cardiac monitoring, backup temporary pacing
and ultimately insertion of a permanent pacemaker.
Second Degree AV Block Vs SVT
++AV
Block:Second Degree, “Fixed Ratio” Blocks++
Fixed
Ratio AV blocks
*Second
degree heart block with a fixed ratio of P waves: QRS complexes (e.g. 2:1, 3:1,
4:1).
*Fixed
ratio blocks can be the result of either Mobitz I or Mobitz II conduction.
Mobitz
I or II?
*It
is not always possible to determine the type of conduction disturbance
producing a fixed ratio block, although clues may be present.
*Mobitz
I conduction is more likely to produce narrow QRS complexes, as the block is
located at the level of the AV node. This type of fixed ratio block tends to
improve with atropine and has an overall more benign prognosis.
*Mobitz
II conduction typically produces broad QRS complexes, as it usually occurs in
the context of pre-existing LBBB or bifascicular block. This type of fixed
ratio block tends to worsen with atropine and is more likely to progress to 3rd
degree heart block or asystole.
*However,
this distinction is not infallible. In approximately 25% of cases of Mobitz II,
the block is located in the Bundle of His, producing a narrow QRS complex.
Furthermore, Mobitz I may occur in the presence of a pre-existing bundle branch
block or interventricular conduction delay, producing a broad QRS complex.
*The
only way to be certain is to observe the patient for a period of time (e.g.
watch the cardiac monitor, print a long rhythm strip, take serial ECGs) and
observe what happens to the PR intervals. Often, periods of 2:1 or 3:1 block
will be interspersed with more characteristic Wenckebach sequences or runs of Mobitz
II.
++High
Grade AV Block++
High
Grade AV Block Definition
*Second
degree heart block with a P:QRS ratio of 3:1 or higher, producing an extremely
slow ventricular rate.
*Unlike
3rd degree heart block there is still some relationship between the P waves and
the QRS complexes.
*High-grade
AV block may result from either Mobitz I or Mobitz II AV block.
Complete
Heart Block (CHB) Overview
*In
complete heart block, there is complete absence of AV conduction – none of the
supraventricular impulses are conducted to the ventricles.
*Perfusing
rhythm is maintained by a junctional or ventricular escape rhythm.
Alternatively, the patient may suffer ventricular standstill leading to syncope
(if self-terminating) or sudden cardiac death (if prolonged).
*Typically
the patient will have severe bradycardia with independent atrial and
ventricular rates.
Mechanism
*Complete
heart block is essentially the end point of either Mobitz I or Mobitz II AV
block.
*It
may be due to progressive fatigue of AV nodal cells as per Mobitz I (e.g.
secondary to increased vagal tone in the acute phase of an inferior MI).
*Alternatively,
it may be due to sudden onset of complete conduction failure throughout the
His-Purkinje system, as per Mobitz II (e.g. secondary to septal infarction in
acute anterior MI).
*The
former is more likely to respond to atropine and has a better overall
prognosis.
Causes Of Complete Heart Block
The
causes are the same as for Mobitz I and Mobitz II second degree heart block.
The most important aetiologies are:
*Inferior
myocardial infarction
*AV-nodal
blocking drugs (e.g. calcium-channel blockers, beta-blockers, digoxin)
*Idiopathic
degeneration of the conducting system (Lenegre’s or Lev’s disease)
Clinical Significance
*Patients
with third degree heart block are at high risk of ventricular standstill and
sudden cardiac death.
*They
require urgent admission for cardiac monitoring, backup temporary pacing and
usually insertion of a permanent pacemaker.
Complete
Heart Block Should Not Be Confused With
*High
grade AV block: A type of severe second degree heart block with a very slow
ventricular rate but still some evidence of occasional AV conduction.
PAC Vs Junctional Rhythm
Inverted P Wave
*P-wave
inversion in the inferior leads indicates a non-sinus origin of the P waves.
*When
the PR interval is < 120 ms, the origin is in the AV junction (e.g.
accelerated junctional rhythm).
*When
the PR interval is ≥ 120 ms, the origin is within the atria (e.g. ectopic
atrial rhythm).
Multiple P Wave Morphologies
Multiple P Wave Morphologies
*The
presence of multiple P wave morphologies indicates multiple ectopic pacemakers
within the atria and/or AV junction.
*If
≥ 3 different P wave morphologies are seen, then multifocal atrial rhythm is
diagnosed.
*If
≥ 3 different P wave morphologies are seen and the rate is ≥ 100, then
multifocal atrial tachycardia (MAT) is diagnosed.
P Pulmonale
Right Atrial Enlargement-Lead
II
*In
right atrial enlargement, right atrial depolarisation lasts longer than normal
and its waveform extends to the end of left atrial depolarisation.
*Although
the amplitude of the right atrial depolarisation current remains unchanged, its
peak now falls on top of that of the left atrial depolarisation wave.
*The
combination of these two waveforms produces a P waves that is taller than
normal (> 2.5 mm), although the width remains unchanged (< 120 ms).
Right Atrial
Enlargement-Lead V1
*Right
atrial enlargement causes increased height (> 1.5mm) in V1 of the initial
positive deflection of the P wave.
P Mitrale
Left Atrial Enlargement-Lead
II
*In
left atrial enlargement, left atrial depolarisation lasts longer than normal
but its amplitude remains unchanged.
*Therefore,
the height of the resultant P wave remains within normal limits but its
duration is longer than 120 ms.
*A
notch (broken line) near its peak may or may not be present (“P mitrale”).
Left Atrial
Enlargement-Lead V1
Left
atrial enlargement causes widening (> 40ms wide) and deepening (> 1mm
deep) in V1 of the terminal negative portion of the P wave.
Biatrial Enlargement
*Biatrial
enlargement is diagnosed when criteria for both right and left atrial
enlargement are present on the same ECG.
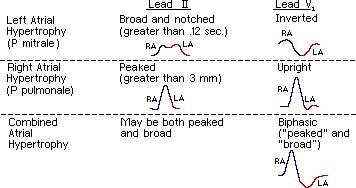
*The
spectrum of P-wave changes in leads II and V1 with right, left and bi-atrial
enlargement is summarised in the following diagram.
*Common
P Wave Abnormalities.
Common
P Wave Abnormalities
*P
mitrale (bifid P waves), seen with left atrial enlargement.
*P
pulmonale (peaked P waves), seen with right atrial enlargement.
*P
wave inversion, seen with ectopic atrial and junctional rhythms.
*Variable
P wave morphology, seen in multifocal atrial rhythms.
Wolff-Parkinson-White Syndrome Pre Excitation Atrial Fibrillation
Wolff-Parkinson-White Syndrome With Delta Wave
++PR Interval++
*The
PR interval is the time from the onset of the P wave to the start of the QRS
complex.
*It
reflects conduction through the AV node.
*The
normal PR interval is between 120 – 200 ms duration (three to five small
squares).
*If
the PR interval is > 200 ms, first degree heart block is said to be present.
*PR
interval < 120 ms suggests pre-excitation (the presence of an accessory
pathway between the atria and ventricles) or AV nodal (junctional) rhythm.
*Type
Of AV Block has been describe above.
Short PR interval
(<120ms)
A
short PR interval is seen with:
*Preexcitation
syndromes.
*AV
nodal (junctional) rhythm.
Wolff-Parkinson-White
(WPW) And Lown-Ganong-Levine (LGL) Syndromes.
*These
involve the presence of an accessory pathway connecting the atria and
ventricles.
*The
accessory pathway conducts impulses faster than normal, producing a short PR
interval.
*The
accessory pathway also acts as an anatomical re-entry circuit, making patients
susceptible to re-entry tachyarrhythmias.
*Patients
present with episodes of paroxsymal supraventricular tachycardia (SVT),
specifically atrioventricular re-entry tachycardia (AVRT), and characteristic
features on the resting 12-lead ECG.
Wolff-Parkinson-White Syndrome
*The
characteristic features of Wolff-Parkinson-White syndrome are a short PR
interval, broad QRS and a slurred upstroke to the QRS complex, the delta wave.
*Short
PR (<120ms), broad QRS and delta waves in WPW syndrome
Wolff
-Parkinson- White Syndrome Cases Usually
*ECG
pattern depends on where the accessory pathway inserts.
Classically:
*Short
PR interval <120 msecs.
*QRS
> 100msecs.
*Delta
wave-slurred upstroke at beginning of QRS.
Different
insertions:
*Normal
QRS if pathway inserts into infranodal conduction tissue just below AV node
*Grossly
wide and abnormal QRS if pathway inserts into non-conduction tissue.
Key
Management Points For WPW
*A
heart rate ≥ 200 should make you think of a pre-excitation syndrome.
*Narrow
complex SVT is treated identically to non-WPW SVT.
*Don’t
try and be clever with drugs in broad complex tachycardias and WPW.
*Using
AV nodal blockers in WPW and AF can result in 1:1 conduction to the ventricles.
*This
is also know as Ventricular Fibrillation.
*Just
shut-up + DC cardiovert them.
Lown-Ganong-Levine Syndrome
*The
features of LGL syndrome are a very short PR interval with normal P waves and
QRS complexes and absent delta waves.
*Short
PR interval with normal QRS complexes in LGL syndrome
AV Nodal (Junctional) Rhythm
*Junctional
rhythms are narrow complex, regular rhythms arising from the AV node.
*P
waves are either absent or abnormal (e.g. inverted) with a short PR interval (retrograde
P waves).














Hi Admin!
ReplyDeleteYour information is very useful for us. Thanks for sharing informational blog post. Keep it up. For more information click this hyperlink QRS Complex
ReplyDeleteNatural herbs can cure epilepsy & haemochromatosis disease, I had epilepsy & haemochromatosis for over 14 years, i have spent a lot money getting drugs from the store to keep me healthy, I went to many hospitals for cure but there was no solution, One day I was in the office going through the internet when I saw a post about Dr Itua herbal medicine on how he cure a Lady from Kansas who was suffering from prostate cancer and she listed Epilepsy as list of illness Dr Itua can as well cured I contacted him with epilepsy Cure solution, I email him. He told me the things I needed to do and also gave me instructions to take, which I followed properly. Before I knew what is happening after two weeks To my greatest surprise after patiently going according to instruction given to me by Dr Itua, my epilepsy was cure, I want to say a big thanks to Dr Itua who God have sent to heal his people with his natural medicine I pray that God will bless you for the good work you are doing.for all who are still suffering from this illness, you can also contact him through his email on :;;drituaherbalcenter@gmail.com Or visit his website to read more about his herbal medicines...www.drituaherbalcenter.com like they say his herbal remedy is the only permanent solution to Seizure. He Can as well cure the following... Herpes Virus, HIV/Aids, Hepatitis A/B, haemochromatosis diseases,Shingles, Cold Sore, Epilepsy, Wart, Lupus, Diabetes, Men/Woman Infertility, Seizure, Cancer all types.